Surgeries range from minor repairs lasting only minutes to major, life-saving operations that take several hours to complete. While the surgeon is the main player in the operating room, he or she is only one of the members of a surgical team. Depending on the hospital and type of surgery, this team may include an anesthesiologist, a certified registered nurse anesthetist, an operating room nurse, and a physician assistant. All work together to ensure a smooth and safe operation.
But there's another team member, one who directly affects how well the surgeon is equipped for the job at hand. Meet the surgical technologist.
Day in The Life of a Surgical Tech
The surgical technologist, also known as a surgical tech, is a skilled professional that makes sure the necessary materials and surgical instruments are prepped and ready to go before the surgeon arrives. During the procedure, the surgical tech retrieves those materials and instruments the moment the surgeon calls for them. And after the surgery, the surgical tech disposes of used materials and sends instruments to be sterilized. It's a demanding, detail-oriented job-and an important one. When it comes to ensuring a sterile operating environment, surgical techs are on the front line.
Picture yourself a surgical tech. Here's what a typical day on the job might look like.
Preoperative Surgical Tech Responsibilities
Your schedule may vary, but you're likely working full time, sometimes with shifts more than 8 hours long, and possibly on call. You're the first team member to enter the operating room. And since morning surgeries are usually preferred, chances are you're up early and probably eating breakfast on the go. While some hospitals provide scrubs and changing facilities, others do not, so you might have to wear your own scrubs to work.
After arriving at the hospital, you head toward the charge nurse's desk. There, you check the list of scheduled cases-or patients undergoing surgery-and which operating room you're assigned to. You then attend a briefing where the surgical team discusses the operation. You're given a preference card, which lists the surgeon's expectations and the exact materials and instruments needed for the case. Next, you visit the sterile supply room, grab a case cart, and load it with the items listed on the preference card.
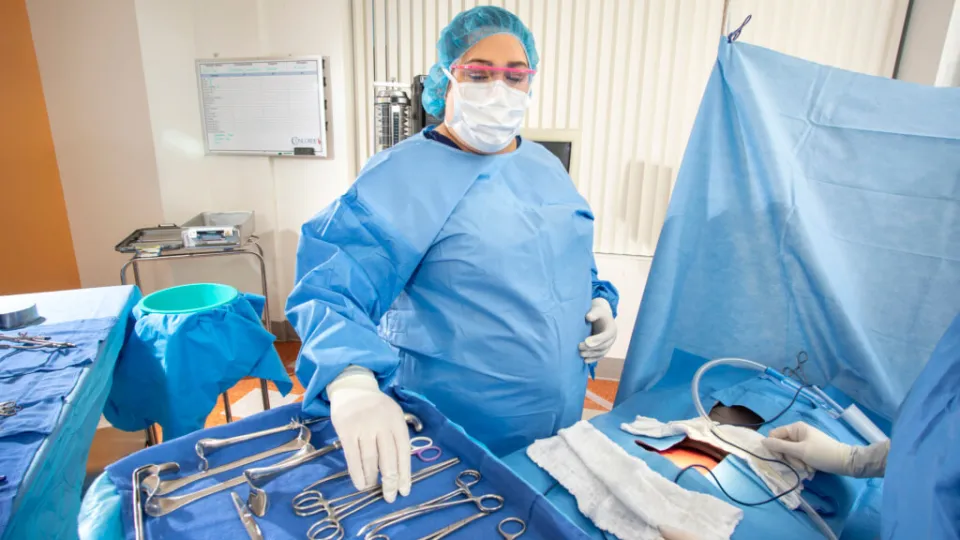
Now you're ready for the operating room-but don't forget to put on your surgical mask before entering. You know that infection-causing germs can be introduced any time protocol is ignored. The area you're working in during surgery is a sterile field into which microorganisms must not enter. After rolling your case cart into position, you "scrub in." This involves removing jewelry and thoroughly washing your hands and forearms, then donning your surgical gown and gloves.
Once suited up, you begin setting up the surgical instruments (clamps, forceps, hemostats, retractors, scissors, etc.) and disposable materials (blades, electrocautery tips, laparotomy pads, needles, suction tubing, sutures, etc.). As you unpackage and lay these onto the surgical tray, you'll count each item while the circulating nurse observes and documents the count. All instruments and materials must be accounted for before, during, and after surgery.
At last, the surgeon arrives and the patient is checked in. The case can begin. You may be asked to gown and glove the surgeon and other team members after they scrub in. You will probably help cover the patient with surgical drapes.
Intraoperative Surgical Tech Responsibilities
During the operation, you anticipate the surgeon's next moves and have the needed instruments and supplies ready to pass. Of course, you are familiar with all of the instruments and can quickly tell the difference between, for example, an Allis clamp and a Duval clamp.
The surgeon may call on you to measure medications, to suction or sponge out the wound, hold instruments in place during the procedure, and cut sutures. For endoscopic surgery, you may be responsible for manipulating the camera. Once the incision has been closed, you'll prepare and apply sterile bandages.
Postoperative Surgical Tech Responsibilities
When the operation is finished and all surgical instruments and materials have been counted, you'll throw away disposable items and prepare the reusable instruments for sterilization. If anything was left off of the surgeon's preference card, you as the surgical tech will make the surgeon's future cases more efficient by adding those details to the document. Now, it's on to the next case.
According to the Bureau of Labor Statistics, surgical tech positions typically require an associate's degree or a postsecondary non-degree award. Surgical techniques are constantly improving, which means opportunities in the field will likely grow. Job openings for surgical techs are expected to increase by 9% over the next decade, also according to the Bureau of Labor Statistics.
Concorde Career College offers an Associate degree in Surgical Technology. Nine of our thirteen campuses are accredited by the Commission on Accreditation of Allied Health Education Programs (CAAHEP), and the program prepares students for entry-level positions in the field of Surgical Technology. Students may take courses at one of 13 campuses across the United States, or complete the online degree completion program from the comfort of their home. For more information, contact Concorde today.
Interested In How To Become a Surgical Tech?
Click here to explore Surgical Technology Programs near you!
Take The Next Step Towards a Brighter Future
Interested in learning more about our Surgical Technology program?
We have a Concorde representative ready to talk about what matters most to you. Get answers about start dates, curriculum, financial aid, scholarships and more!