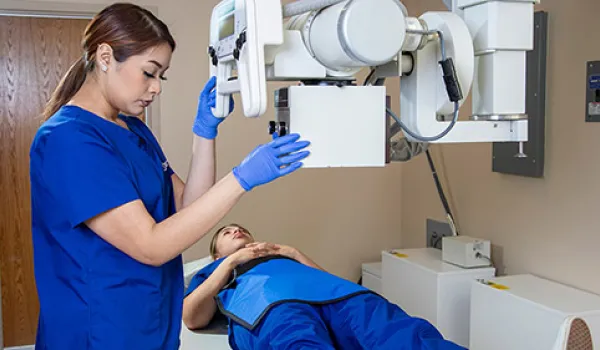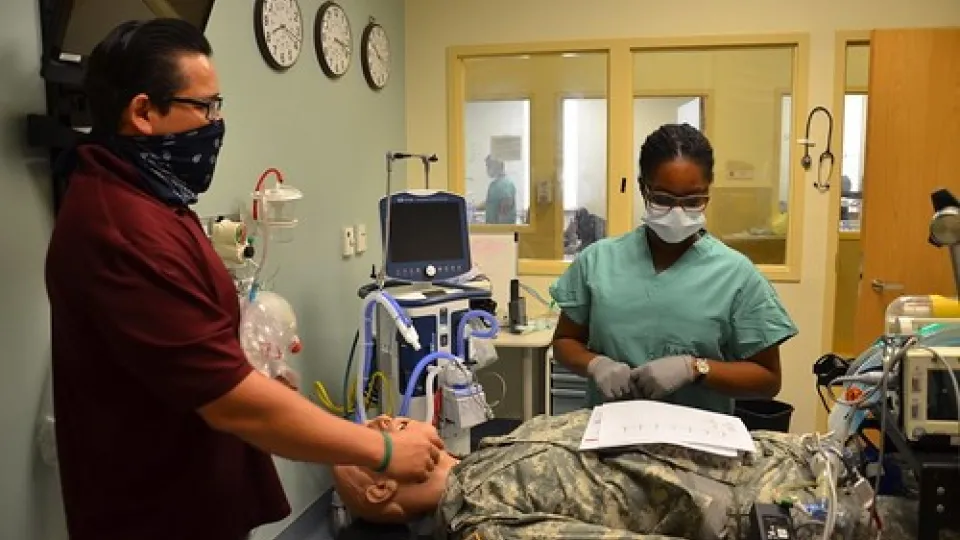
Respiratory therapy is a rapid-growing form of health care because it covers an extensive range of breathing-related conditions, from asthma to lung cancer (1). Therefore, the respiratory therapy field can offer plenty of career options for aspiring health care professionals. Additionally, respiratory therapy provides an exceptional opportunity to help others. The duties and responsibilities of a respiratory therapist (RT) can vary greatly depending on the specialization. Find out what types of conditions an RT treats in the following comprehensive guide.
What Does a Respiratory Therapist Do?
In general, an RT's job involves diagnosing, treating, managing, and helping to prevent breathing and other cardiopulmonary disorders. RTs can help patients with all types of respiratory conditions, from blocked air passageways to pneumonia. Some of the conditions that respiratory therapists treat can be life-threatening conditions, such as an intense asthma attack or lung cancer. Typically, an RT's daily activities include evaluating new patients, treating and following up with existing patients, and documenting patient progress.
RTs work in various health care settings, such as clinics, hospitals, physicians' offices, emergency rooms, critical care units, neonatal intensive care units, sleep centers, and patients' homes (2). In many cases, they're full-time professionals. Those who work in medical facilities that are always open may sometimes work at night or during weekends.
What Types of Conditions Do Respiratory Therapists Treat?
RTs work closely with physicians and nurses to devise appropriate treatment plans for patients. These individuals are involved in treating breathing and airway issues that can result from an array of conditions such as the following:
Chronic Obstructive Pulmonary Disease (COPD)
As one of the most common and fatal chronic respiratory conditions, COPD is a progressive lung disease that causes breathing difficulty (3). COPD is an umbrella term used for long-term lung conditions such as:
- Emphysema: Emphysema is a disease that results from damaged air sacs in the lungs. Once the disease destroys the air sacs' walls, the air sacs merge into one large air sac and lose their ability to absorb oxygen properly. Consequently, less oxygen is present in the blood. Damaged air sacs can make the lungs stretch out and become less springy. With air trapped in their lungs, people who suffer from emphysema have difficulty exhaling.
- Chronic bronchitis: Chronic bronchitis is a condition that causes a person to experience shortness of breath, coughing, and excessive mucus. It results in the loss of cilia, which are hair-like fibers that line the bronchial tubes and help remove mucus. Since it hinders mucus clearance, this condition leads to coughing and the production of more mucus.
- Refractory asthma: Asthma patients are regarded as refractory when they have persistent symptoms, frequent asthma attacks, and poor lung function even though they're taking asthma medications. This condition is sometimes called nonreversible asthma.
COPD may occur because of a variety of factors. The most common causes of this condition are smoking and exposure to secondhand smoke, dust, air pollution, and certain chemicals. Also, asthma patients are at a higher risk of developing the disease. COPD often doesn't have noticeable signs in its early stages, but it may present the following symptoms as it worsens:
- Chronic coughing.
- Coughing up excessive mucus.
- Wheezing or squeaking while breathing.
- Shortness of breath, especially during physical activity.
- Tightness in the chest.
- Frequent colds.
- Fatigue.
- Swollen legs, ankles, and feet.
- Blue fingernails.
- Unintentional weight loss.
When treating COPD, an RT typically starts by asking questions about the patient's symptoms, medical history, and exposure to risk factors such as tobacco smoke, dust, and chemicals. An RT will conduct a physical exam and breathing test. The most common breathing test is spirometry, which measures the amount of air the lungs can hold and the speed at which the patient can expel air from the lungs. A COPD diagnosis may also include lung function tests, chest X-rays, CT scans, and arterial blood gas tests.
While no cure for COPD exists, treatment aims to ease the symptoms and slow down the disease. RTs may use an array of methods to treat or prevent complications, such as the following:
- Bronchodilators.
- Corticosteroids.
- Combination inhalers.
- Roflumilast.
- Antibiotics.
- Oxygen therapy.
- Pulmonary rehabilitation.
Asthma
Asthma refers to a condition in which the airways are swollen and narrow and produce more mucus than usual. This condition may cause shortness of breath and coughing. The disease can range from a minor nuisance to a significant issue that interferes with day-to-day activities. An asthma attack can be a potentially life-threatening medical event.
The symptoms of asthma vary from one person to another. A patient may experience symptoms only during exercise, have occasional asthma attacks, or display symptoms all the time. Below are the most common signs and symptoms of asthma:
- Breathing difficulty.
- Chest pain or tightness.
- Wheezing during exhalation.
- Coughing and wheezing attacks, especially when having a cold or flu.
- Trouble sleeping because of shortness of breath, wheezing, or coughing.
While medical professionals can't completely cure this respiratory condition for patients, they can help patients control the symptoms. An RT will evaluate a patient's medical history and perform a physical exam to diagnose this condition. Testing may involve the following:
- A lung function test.
- Chest or sinus X-ray.
- Methacholine test.
- Allergy test.
- Nitric oxide test.
- Provocative test.
Usually, asthma treatment involves learning how to recognize and avoid triggers by using the correct medications and quick-relief inhalers. Monitoring breathing becomes necessary to ensure the medications are effective in keeping symptoms under control. Some of the medicines commonly used for managing asthma include:
- Inhaled corticosteroids.
- Oral and intravenous corticosteroids.
- Leukotriene modifiers.
- Combination inhalers.
- Theophylline.
- Anticholinergic agents.
- Short-acting beta-agonists.
- Allergy shots.
Acute Bronchitis
Besides treating long-term cardiorespiratory conditions, an RT may also help people overcome acute respiratory diseases such as acute bronchitis. Acute bronchitis is a short-term condition that causes the breathing tubes or airways to experience inflammation, leading to increased mucus production, coughing, and other symptoms. Also referred to as a chest cold, this illness usually results from the same viral infection that causes colds and the flu. It can also occur because of a bacterial infection or exposure to harmful physical or chemical agents such as dust, allergens, tobacco smoke, strong fumes, and chemical compounds.
In most cases, acute bronchitis doesn't last more than two weeks (4). However, some patients may experience coughing for up to eight weeks. The following are the symptoms of this condition:
- Excessive mucus.
- Coughing.
- Chills.
- Runny nose.
- Sore throat.
- Slight fever.
- Watery eyes.
- Shortness of breath.
- Wheezing.
- Headache.
- Fatigue.
- Chest soreness.
- Back and muscle pain.
Generally, an RT will often review a medical history or conduct a physical exam to diagnose acute bronchitis. An RT may also perform several of the following tests to rule out asthma, pneumonia, and other similar conditions:
- Chest X-ray.
- Arterial blood gas test.
- Pulse oximetry.
- Nasal discharge or sputum test.
- Pulmonary function test.
Acute bronchitis is a mild condition that rarely leads to complications. The symptoms often go away on their own, and lung function returns to normal within two weeks (5). Usually, treatment of this illness doesn't involve the use of antibiotics. Some of the methods of treating acute bronchitis include:
- Cough medicine.
- Pain relievers.
- Fever reducers.
- Air humidification.
- Increased fluid intake.
- Quitting smoking or reducing exposure to secondhand smoke.
Pneumonia
Pneumonia is a lung infection that causes the air sacs in the lungs to fill with fluid or pus. This condition can make it difficult for a person to inhale sufficient oxygen to reach the bloodstream. Pneumonia can range from a mild illness to a severe disease that leads to hospitalization. Anyone can contract this lung infection, but infants and older adults are especially susceptible. Several factors can contribute to the development of pneumonia, including bacterial or viral infection, smoking, and excessive alcohol consumption.
Pneumonia symptoms may differ depending on the condition's cause and a patient's age and overall health. These symptoms usually develop over a few days, but they may not be obvious (6). Common pneumonia symptoms include:
- Coughing that produces mucus or phlegm.
- Chest pain while breathing or coughing.
- Shortness of breath.
- Fatigue.
- Loss of appetite.
- Sweating.
- Chills.
- Fever.
- Nausea.
- Vomiting.
- Diarrhea.
To determine whether a person has pneumonia, an RT will first try to learn about the individual's symptoms and medical history, such as whether the person has been around sick people at home or at work and whether the patient has a smoking habit. Listening to the lungs is an effective way to identify pneumonia because those suffering from the condition may produce bubbling, rumbling, or crackling sounds when breathing. Additionally, an RT may perform a variety of tests to confirm the diagnosis of pneumonia, such as:
- Blood test.
- Sputum test.
- Pulse oximetry.
- Arterial blood gas test.
- Pleural fluid test.
- Chest X-ray.
- CT scan.
- Bronchoscopy.
After a pneumonia diagnosis, the RT will work with a doctor to develop a treatment plan. The treatment method depends on the type of pneumonia affecting the patient. People who have bacterial pneumonia usually take antibiotics, while those with viral pneumonia may need to take fever medicine, drink plenty of fluids, and rest. If the symptoms are severe, an individual may require hospitalization.
Sinusitis
Also known as a sinus infection, sinusitis is one of the most prevalent upper respiratory conditions. This type of infection is an inflammation of the sinuses and nasal passages. Located behind the forehead and nose and between the eyes, sinuses are tiny air pockets that produce mucus to trap and remove germs. When exposed to bacteria or allergens, they may generate too much mucus, which blocks their openings and leads to breathing difficulty.
Acute sinusitis typically goes away on its own within four weeks, while subacute sinusitis can last for up to three months. Chronic sinusitis may last for more than three months, but its symptoms are often milder (7). All types of sinusitis have the same symptoms, which include the following:
- Runny or stuffy nose.
- Reduced sense of smell.
- Coughing.
- Fever.
- Headache.
- Fatigue.
An RT can diagnose sinusitis by asking patients about their symptoms and doing a physical exam. However, they may perform an additional test, such as a CT scan, an MRI, a fiber-optic endoscopic evaluation, or an allergy test, if they suspect the infection is chronic. An RT can treat sinusitis in several ways, including nasal saline rinses, mucus-thinning medication, corticosteroid nasal spray, antibiotics, and surgery.
How To Become a Respiratory Therapist

How To Become a Respiratory Therapist
Becoming an RT is an exciting and rewarding career path. You'll have the opportunity to help countless patients improve their quality of life throughout your career. To become certified as an RT, you must possess at least an associate degree and pass the Certified Respiratory Therapist (CRT) or Registered Respiratory Therapist (RRT) exam. Also, all states except Alaska require licensing (8). Accredited RT programs include primary education and hands-on training to enable you to perform an RT's duties thoroughly.
Besides an associate degree and professional certification, specific abilities and traits to excel in the field of respiratory therapy are recommended. These traits include interpersonal skills, compassion, patience, science and math skills, and problem-solving skills.
Related: Prerequisites For Respiratory Therapy Programs
Apply for the Respiratory Therapy Program at Concorde Career College
At Concorde Career College, our Respiratory Therapy Associate Degree program is designed to help aspiring RTs gain the knowledge and skills needed to become a CRT or RRT, including chest physiotherapy, oxygen therapy, bronchodilation, and electrocardiography. This program leads to an associate degree and includes educational preparation for a respiratory therapy career in 18 months or more. We have 12 campuses across the country offering this accredited respiratory therapy program, including Garden Grove, San Antonio, Kansas City, Portland, and Tampa.
Contact us today to find out about our admission requirements, curriculum, and course schedules.
Interested In How To Become a Respiratory Therapist?
Click here to explore Respiratory Therapy Programs near you!
Footnotes:
li>"Image" 502 ABW/PA, https://www.flickr.com/photos/jbsapublicaffairs/50744343127/sizes/m/
"COVID-19 Pandemic Sees Growing Demand for Respiratory Therapists," Spectrum News, https://spectrumlocalnews.com/nys/rochester/health/2020/09/24/growing-demand-for-respiratory-therapists-amid-covid-19
"What Is a Respiratory Therapist?" WebMD, https://www.webmd.com/lung/what-respiratory-therapist
"A Patient's Guide to Respiratory Disease," U.S. News & World Report, https://health.usnews.com/conditions/respiratory-disease
"How Long Do Symptoms of Bronchitis Last?" Healthline, https://www.healthline.com/health/how-long-does-bronchitis-last
"Acute Bronchitis," Familydoctor.org, https://familydoctor.org/condition/acute-bronchitis/
"Pneumonia Symptoms and Diagnosis," American Lung Cancer, https://www.lung.org/lung-health-diseases/lung-disease-lookup/pneumonia/symptoms-and-diagnosis
"What You Need to Know About Sinusitis," Healthline, https://www.healthline.com/health/sinusitis
"Respiratory Therapists," U.S. Bureau of Labor Statistics, https://www.bls.gov/ooh/healthcare/respiratory-therapists.htm
Take The Next Step Towards a Brighter Future
Interested in learning more about our Respiratory Therapy program?
We have a Concorde representative ready to talk about what matters most to you. Get answers about start dates, curriculum, financial aid, scholarships and more!