Written by Jeanette Robins, BS Director of Concorde's Polysomnographic Technology Program and Neurodiagnostic Technology Program in Grand Prairie.
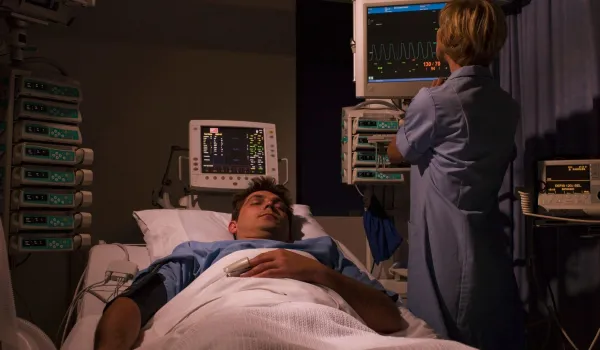
Neurodiagnostic Technologists (NDTs) often work in hospitals or outpatient centers. However, there are some who find themselves in research facilities or laboratories. In "sleep labs," NDTs are part of a scientific team conducting studies in narcolepsy, parasomnias or insomnia. Whether in a lab or as part of a hospital, NDTs interact directly with patients and will provide important data results to physicians. The test results and their interpretation can help identify and diagnose neurological conditions like epilepsy, Parkinson's disease and multiple sclerosis.
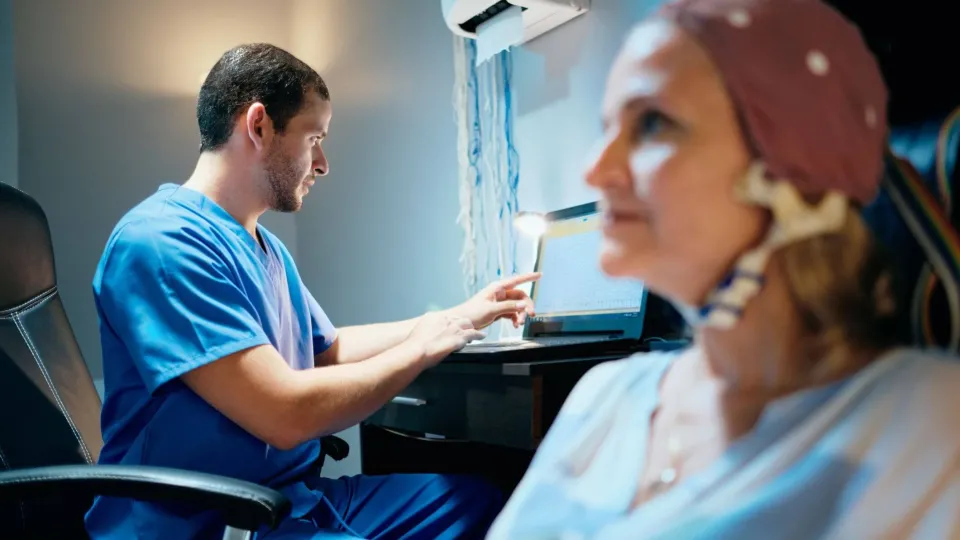
Neurodiagnostic techs administer and interpret different types of neurological tests each day. These tests are intended to understand a patient's brain waves. They are critical in understanding a patient's neurology; focusing on the brain, spinal cord, and nervous system. Becoming an NDT requires a meticulous and inquisitive nature, as well as an interest in complex technology - beginning with the human brain.
A Professional Prospective
To understand what it's like to be a Neurodiagnostic Technologist, it's helpful to get a personal perspective from a variety of Neurodiagnostic Technologists currently working in the field at varying levels in their career. Depending upon their years of experience and specialization area, their day comes with a routine that is part of a fulfilling career.
Alfredo Hernandez, R.EEG T., R.NCS.T., REPT, and Concorde NDT instructor, describes his day at the Medical Center; "I arrive each morning and check the queue for pending orders, followed by an 8:30 skype meeting where different department sections give updates on their caseloads. If a department section needs assistance, and we are not then we will spend the day helping them. Throughout the day, it is common to find the senior tech helping the junior tech prepare for more advance neurological studies and even help them study for their board exam. When we do have orders, then we contact the ordering physician's nurse to coordinate the patient's study.
There are plenty of reasons why I love my job. It appeals to my nerdy personality, because you really need to know what you are doing (lots of reading and studying) It goes beyond just performing the study, we are an essential part of the diagnostic team. As a Neuro Tech, I must be ready to alert a doctor to critical findings, as when the patient is in subclinical status. We can make a big difference in patient outcomes by recognizing and immediately calling the doctors instead of leaving the study to be read later."
Ana Raicu, R.EEG T., R.NCS.T., CNIM, and Concorde NDT Clinical Director, shares what her days include at the hospital: "My job is to test the central and peripheral nervous system applying a variety of tools and advanced testing methods."
As an NDT, I may use:
- Electroencephalograms - record brain activity, similarly to an EKG recording that measure the heart's electrical activity
- Nerve Conduction Studies - record peripheral nerves' responses to electrical stimulation
- Interoperative monitoring - record the nervous system activity during brain and spine surgeries
- Evoked Potentials - record brain response to peripheral nerve stimulation
"After 20 years working in the neurodiagnostic field I am still passionate about it. I love caring for patients and working in health care. Even if the human body doesn't change during a lifetime, the technology used in health care is advancing constantly and rapidly. Newer more efficient tools are at our disposal to test and treat patients. Technology nerds are having a blast working in NDT."
A Recent Graduate Prospective
In contrast, recent Concorde NDT graduate Darnequitta Chambers' day starts off at Ochsner LSU Health Shreveport Neurology Department setting up the "cart"of supplies she'll need for her scheduled procedures. "My setup procedure is routine so that I am ready. I then log into the hospital system to see which patients are assigned to me. I roll my cart with the electroencephalogram (EEG) equipment and supplies to the patient. It's important that I begin by explaining the prescribed procedure, it helps calm the patient's fears. I'll answers questions, perform the study, clean- up and head back to my office to wait for the next patient.
The main reason people are sent to me is because they've experienced a seizure. I'm pretty much everywhere in the hospital, I have even been called into the newborn intensive care unit (NICU). Personally, I like the Epilepsy Monitoring Unit (EMU) the best."
Not everything goes according to plan. "Recently one of my patients in the intensive care unit (ICU) had too much muscle artifact, so the study was not readable. After consulting with the patient's care team, the patient was given medication to relax. At which point I was able to retest and record the required brain activity."
For Darnequitta, her career path is personal; "I am so glad that I went into this field because my daughter was having sleep apnea. So, I understood the impact that can have on her physically and emotionally. I wanted a career that would allow me to help others with these types of conditions. I feel fulfilled and can make a good living at this," she said.
Continuing to Grow
Our understanding of the human brain continues to expand. We have come a long way in our ability to map and track how the brain responds to stimuli or from trauma. Whether helping diagnose disease, impact injury, sleep patterns or aid in the treatment or repair, Neurodiagnostic Technologists play an important role in health care.
An associate degree through a Neurodiagnostic Technology program, which can be completed in as few as 17 months at a school like Concorde, can prepare you for entry into the field. A dream career in health care could begin in Neurodiagnostic Technology.
Interested In How To Become a Neurodiagnostic Technologist?
Click here to explore Neurodiagnostic Technology Programs near you!
About the Author
Jeanette currently serves as the NDT/PSG Program Director at Concorde Career Colleges, Grand Prairie and has been with Concorde since June 2016. She previously directed Sleep and EEG programs for over 20 years in clinics. She worked on the curriculum committee at Weber State University to help create their Bachelor's in Respiratory Therapy program by adding in a PSG diploma, and served as adjunct faculty for many years.
She received her Bachelor of Science degree from BYU and has been a Registered Polysomnographic Technologist since 1997. She has served as the National Education Chair for the AAST (American Academy of Sleep Technologists), and as a Liaison in Washington DC for the National Sleep Awareness Roundtable.
Take The Next Step Towards a Brighter Future
Interested in learning more about our Neurodiagnostic Technology program?
We have a Concorde representative ready to talk about what matters most to you. Get answers about start dates, curriculum, financial aid, scholarships and more!